Glossary
Induced pluripotent stem cells
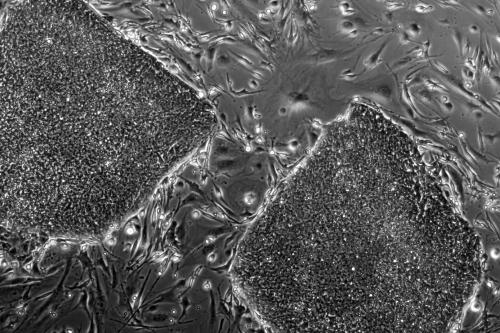
iPSCs are adult cells — typically skin or blood — that have been reprogrammed in the lab to behave like stem cellsCells that have the ability to differentiate into multiple types of cells and make an unlimited number of copies of themselves.stem cellsCells that have the ability to differentiate into multiple types of cells and make an unlimited number of copies of themselves., giving them the potential to become any of the cell types found in all major tissues in the body. Because they are made from a patient's own cells, they carry that person's unique genetic code, making them a powerful tool for disease research and personalized medicine
New to stem cell research? Start with our overview of all stem cell types.
What is reprogrammingIn stem cell research, scientists can reprogram cells that have undergone differentiation, such as skin or blood cells, to revert back into an embryonic-like state. The resulting cells are called induced pluripotent stem cells.reprogrammingIn stem cell research, scientists can reprogram cells that have undergone differentiation, such as skin or blood cells, to revert back into an embryonic-like state. The resulting cells are called induced pluripotent stem cells.?
To understand how iPSC reprogramming works, it helps to understand what stem cellsCells that have the ability to differentiate into multiple types of cells and make an unlimited number of copies of themselves.stem cellsCells that have the ability to differentiate into multiple types of cells and make an unlimited number of copies of themselves. naturally do. When a stem cell divides, one of the resulting cells begins the long process of specialization — gradually committing to become a neuron, a blood cell, a liver cell. The other remains a stem cell, preserving the body's reserve. Reprogramming reverses that journey: it instructs a mature, already-specialized cell to forget its identity and return to that earlier, uncommitted state.
How are iPSCs made?
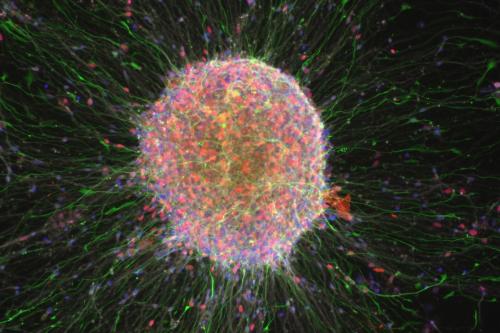
Creating an induced pluripotent stem cell begins with something remarkably ordinary: a small sample of a patient's own skin or blood cells, collected and brought to the laboratory. Scientists introduce a carefully selected set of genes — known as reprogramming factors — that instruct the cell to revert to a pluripotent state. From a single patient sample, scientists can generate an unlimited supply of these cells, then guide them toward becoming neurons, heart muscle cells, liver cells, blood cells, and more.
Why does this matter for patients?
Because iPSCs carry the patient's own genetic code, they offer something embryonic stem cellsPluripotent stem cells that give rise to every cell type in the adult body. They are derived from the inner cell mass of a blastocyst.embryonic stem cellsPluripotent stem cells that give rise to every cell type in the adult body. They are derived from the inner cell mass of a blastocyst. cannot: a perfectly personalized model of that individual's biology. This makes them invaluable not just for studying how diseases develop, but for testing whether a specific therapy will work — or cause harm — in that particular patient.
Diseases We're Studying with iPSC Technology

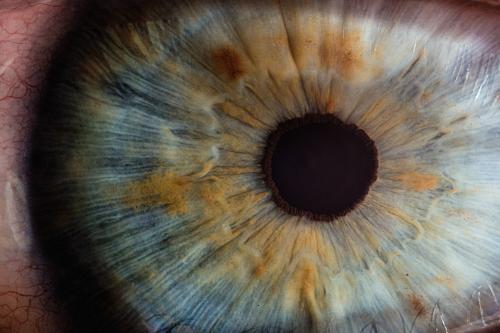
Macular Degeneration & Eye Disease
UCLA scientists were the first in the world to transplant stem cell-derived retinal cells into patients — and are now developing therapies using a patient's own iPSCs to grow replacement retinal cells, potentially restoring vision lost to macular degeneration and related conditions.

Duchenne Muscular Dystrophy
By reprogramming cells from Duchenne patients into muscle precursors, our scientists can study this progressive disease and explore gene-correction approaches.
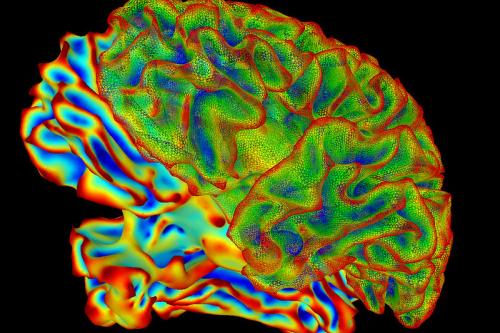
Autism Spectrum Disorder
UCLA researchers use iPSCs from patients with autism to grow miniature brain models in the laboratory — studying the genetic underpinnings of the disorder and identifying potential therapeutic targets.
Alzheimer's Disease
UCLA researchers are using neurons grown from induced pluripotent stem cells to better understand Alzheimer's and related dementias — and to develop new therapies for these devastating diseases.
For Patients & Families
What does iPSC research mean for patients?
If you or someone you love has been affected by a disease that currently has limited treatment options, iPSC research may offer reason for hope. At UCLA, patients and families play an essential role in this work — donating cells that allow our scientists to study diseases in the laboratory and work toward new therapies. We know that research timelines can feel frustratingly slow when you're living with a diagnosis.
Our For Patients & Families page is a resource for understanding where the science stands, what clinical trials may be available, and how to get involved.

Frequently Asked Questions
-
Induced pluripotent stem cells (iPSCs) are created by taking ordinary mature cells from a patient — typically skin or blood — and reprogramming them in the laboratory back to a pluripotent state, meaning they have the potential to differentiate into any of the cell types found in all major tissues in the body. They were first created in 2006 and have since become one of the most important tools in regenerative medicine and disease research.
-
Both iPSCs and human embryonic stem cells (hESCs) are pluripotent — capable of differentiating into a wide range of specialized cell types. The key difference is their origin: hESCs come from donated embryos, while iPSCs are created from a patient's own adult cells. This means iPSCs carry the patient's genetic code, making them useful for personalized disease modeling, and they sidestep many of the ethical concerns associated with embryonic stem cell research.
-
iPSCs are being used to study and develop potential treatments for a wide range of diseases, including macular degeneration and other blinding eye conditions, autism spectrum disorder, Duchenne muscular dystrophy, Lesch-Nyhan syndrome, Alzheimer's disease and other dementias, diabetes and neurological disorders. At UCLA, patients with these and other conditions donate cells to our researchers to enable laboratory modeling of disease.
-
Not yet — but the field is advancing rapidly. As of 2026, no iPSC-based therapy has completed a full three-phase clinical trial and received FDA approval. However, a number of iPSC-derived therapies are currently in clinical trials globally, targeting conditions in neurology, ophthalmology and oncology, and early safety data has been encouraging. At UCLA, the Translational Cell Therapy Lab is specifically focused on moving iPSC discoveries from the laboratory toward clinical application. Visit our For Patients & Families page for information on clinical trials that may be available to you.
-
In late 2007, UCLA researchers Drs. Kathrin Plath, William Lowry, Amander Clark and April Pyle were among the first in the world to create human induced pluripotent stem cells — a landmark discovery that helped establish iPSC research as the foundation for a new era of regenerative medicine.
-
iPSCs can be guided to differentiate into a wide range of cell types. UCLA researchers have successfully reprogrammed cells into motor neurons, liver cells, blood cells, bone precursors, and egg and sperm precursors, among others. Under the right laboratory conditions, iPSCs have the potential to give rise to cell types from all major tissues in the body.
-
There are several ways to support this work: you can donate to the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research at UCLA, participate in research studies if you or a family member has a relevant condition, or stay connected by subscribing to our newsletter for the latest breakthroughs.
-
No. While stem cell research is advancing rapidly, only a small number of stem cell treatments have been rigorously tested and approved for use in patients. A growing number of clinics offer unproven therapies that have not completed the clinical trial process — these can be expensive and, in some cases, carry significant health risks. UCLA is committed to only advancing therapies through proper scientific and regulatory channels. Before considering any stem cell treatment, we encourage patients to visit our For Patients & Families page and consult the International Society for Stem Cell Research's trusted guidance at aboutstemcells.org.