Understanding Stem Cell Research
What's a stem cell?
From the first cell divisions of a developing embryoThe early developmental stage of a multicellular organism, typically occurring after fertilization of an egg cell by a sperm cell.embryoThe early developmental stage of a multicellular organism, typically occurring after fertilization of an egg cell by a sperm cell. to the daily renewal of an aging adult, stem cellsCells that have the ability to differentiate into multiple types of cells and make an unlimited number of copies of themselves.stem cellsCells that have the ability to differentiate into multiple types of cells and make an unlimited number of copies of themselves. are the body's constant, behind-the-scenes workforce.
They sit quietly in reserve throughout your tissues and organs, springing into action when the body needs to replace worn-out cells, repair damage, or build something new.
What makes them uniquely suited to this role is what sets them apart from every other cell in the body — and what has made them one of the most important frontiers in modern medicine.
The foundational building blocks of living organisms, stem cells are defined by two characteristics:
- They can make copies of themselves, or self-renew
- They can differentiate, or develop into more specialized cells
What makes this possible is a kind of elegant self-preservation: when a stem cell divides, the two resulting cells don't always become the same thing. One typically begins specializing into a particular cell type — a neuron, a blood cell, a muscle fiber. The other remains a stem cell, maintaining the body's reserve supply for whenever it's needed again.
In humans, there are different types of stem cells that originate from different parts of the body and emerge during different times in our lives. These include embryonic stem cellsPluripotent stem cells that give rise to every cell type in the adult body. They are derived from the inner cell mass of a blastocyst.embryonic stem cellsPluripotent stem cells that give rise to every cell type in the adult body. They are derived from the inner cell mass of a blastocyst., which only exist during the earliest stages of development, and tissue-specific stem cellsMature stem cells that are found in many adult organs and tissues (such as the brain and muscles). Unlike pluripotent stem cells, they can only produce the cell types found in the organ or tissue they inhabit. They're responsible for replacing cells that have been lost due to natural wear and tear, injury and illness throughout life; however, their ability to do so decreases with age.tissue-specific stem cellsMature stem cells that are found in many adult organs and tissues (such as the brain and muscles). Unlike pluripotent stem cells, they can only produce the cell types found in the organ or tissue they inhabit. They're responsible for replacing cells that have been lost due to natural wear and tear, injury and illness throughout life; however, their ability to do so decreases with age., which arise during fetal development and persist throughout life.
"Stem cells are the foundation of organisms, the stalk from which everything buds and branches.”
Alexander Capron
Bioethicist, World Health Organization
What are the different types of stem cells?
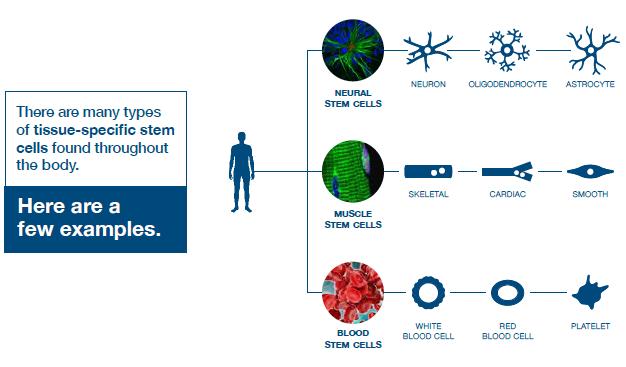
Tissue-Specific Stem Cells
Sometimes referred to as adult or somatic stem cells, these contribute to the body's ability to create new cells that restore damaged organs and tissues. Scientists now know that small populations reside in many organs including the brain, skeletal muscle, skin, heart, intestines and liver. While tissue-specific stem cells help the body repair by producing all the cell types within their designated tissues, their ability to regenerate is limited and decreases over time.
Blood stem cellsA type of tissue-specific stem cells found in the blood and bone marrow that can form various types of mature blood and immune cells. These cells play a crucial role in maintaining the body's blood supply and immune system by continuously producing new blood cells throughout a person's life.Blood stem cellsA type of tissue-specific stem cells found in the blood and bone marrow that can form various types of mature blood and immune cells. These cells play a crucial role in maintaining the body's blood supply and immune system by continuously producing new blood cells throughout a person's life., also known as hematopoietic stem cells, produce all types of blood and immune cells. They’re found in the bone marrow and have been used to treat patients with blood and immune diseases such as leukemia for more than 50 years. Sources for transplantation include bone marrow, umbilical cord blood and peripheral blood.
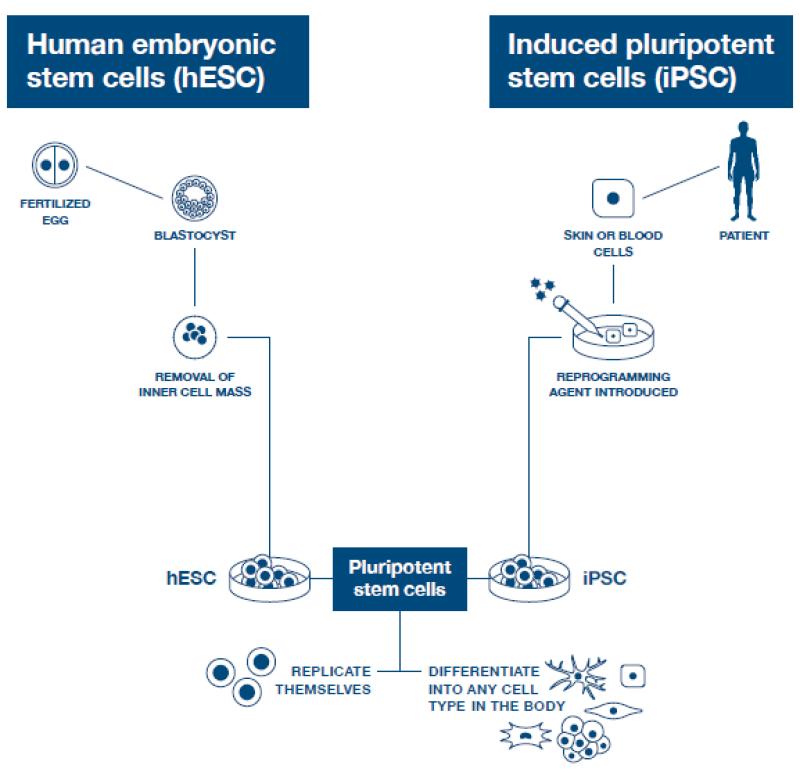
Induced Pluripotent Stem CellsiPSCs are adult cells — typically skin or blood — that have been reprogrammed in the lab to behave like stem cells, giving them the potential to become any of the cell types found in all major tissues in the body. Because they are made from a patient's own cells, they carry that person's unique genetic code, making them a powerful tool for disease research and personalized medicineInduced Pluripotent Stem CellsiPSCs are adult cells — typically skin or blood — that have been reprogrammed in the lab to behave like stem cells, giving them the potential to become any of the cell types found in all major tissues in the body. Because they are made from a patient's own cells, they carry that person's unique genetic code, making them a powerful tool for disease research and personalized medicine (iPSCs)
Induced pluripotent stem cells, or iPSCs, are created by taking ordinary mature cells from a patient — typically skin or blood — and reprogrammingIn stem cell research, scientists can reprogram cells that have undergone differentiation, such as skin or blood cells, to revert back into an embryonic-like state. The resulting cells are called induced pluripotent stem cells.reprogrammingIn stem cell research, scientists can reprogram cells that have undergone differentiation, such as skin or blood cells, to revert back into an embryonic-like state. The resulting cells are called induced pluripotent stem cells. them in the laboratory back to a pluripotent state.
Like embryonic stem cells, they can replicate indefinitely and have the potential to differentiate into any of the cell types found in all major tissues in the body. Because they carry the patient's own genetic code, therapies derived from them could be precisely matched to that individual — minimizing the risk of rejection. UCLA researchers are currently using iPSC technology to model diseases including ALS, Rett syndrome, Duchenne muscular dystrophy and leukemia — work that depends on the generous participation of patients and their families.
In 2006, a team in Japan first demonstrated that this kind of reprogramming was possible. Shortly after, UCLA's own Drs. Kathrin Plath, William Lowry, Amander Clark and April Pyle were the first in California to report successful generation of human iPSCs — and iPSC research at UCLA has been at the forefront ever since.
Human Embryonic Stem CellsPluripotent stem cells that give rise to every cell type in the adult body. They are derived from the inner cell mass of a blastocyst.Embryonic Stem CellsPluripotent stem cells that give rise to every cell type in the adult body. They are derived from the inner cell mass of a blastocyst. (hESCs)
Human embryonic stem cells are pluripotent — meaning they can produce the more than 200 cell types found in the human body through differentiationThe process by which stem cells transform into specific, specialized cell types with distinct functions and features.differentiationThe process by which stem cells transform into specific, specialized cell types with distinct functions and features.. Unlike tissue-specific stem cellsMature stem cells that are found in many adult organs and tissues (such as the brain and muscles). Unlike pluripotent stem cells, they can only produce the cell types found in the organ or tissue they inhabit. They're responsible for replacing cells that have been lost due to natural wear and tear, injury and illness throughout life; however, their ability to do so decreases with age.tissue-specific stem cellsMature stem cells that are found in many adult organs and tissues (such as the brain and muscles). Unlike pluripotent stem cells, they can only produce the cell types found in the organ or tissue they inhabit. They're responsible for replacing cells that have been lost due to natural wear and tear, injury and illness throughout life; however, their ability to do so decreases with age., they can also replicate indefinitely, making them a uniquely powerful and versatile tool for research. Scientists first succeeded in isolating hESCs in 1998, opening a new era in regenerative medicineA field focused on developing and applying new therapies and techniques to repair, replace or regenerate tissues and organs and restore function that has been lost due to aging, disease, injury or genetic defects.regenerative medicineA field focused on developing and applying new therapies and techniques to repair, replace or regenerate tissues and organs and restore function that has been lost due to aging, disease, injury or genetic defects..
Research involving embryonic stem cells is conducted under strict ethical guidelines and oversight through UCLA’s Human Pluripotent Stem Cell Research Oversight (hPSCRO) Committee.
Stem cell research opens doors in medicine that would otherwise remain closed. Because stem cells can become virtually any cell type in the body, scientists can use them to study disease, develop and test treatments, and — in some cases — replace or repair damaged tissue in patients.
6 Ways Stem Cells Advance Biomedical Research
Disease Modeling
Stem cells — particularly iPSCs made from patients — allow scientists to recreate a disease in a laboratory dish, studying how it develops and testing potential therapies without any risk to patients
Drug Discovery & Testing
Researchers use stem cell-derived models to search for new drugs, test how candidate therapies affect different tissues and organs, and predict how individual patients may respond.

Cell Replacement
Scientists are exploring how to use stem cells to generate healthy tissue that, when transplanted, can replace tissue damaged by disease, aging or injury — such as retinal cells lost in macular degeneration.
Personalized Medicine
Patient-specific iPSCs allow researchers to model how an individual's biology responds to different treatments — a step toward therapies tailored to each person's genetic makeup, minimizing rejection risk.
Self-Repair
Scientists are investigating ways to coax the body's own stem cells into generating healthy cells to heal damaged tissue from within, or to prevent further damage before it occurs.
Development & Aging
Stem cells are used to investigate how tissues and organs form, how aging affects their function, and how that knowledge can lead to new treatments for age-related disease.
Framework adapted from the International Society for Stem Cell Research.
Where do we get stem cells for research?
All of the human embryonic stem cells currently used in research come from cell lines that have been approved for research and registered with the National Institutes of Health. The original hESCs used to establish these lines came from embryos donated by consenting individuals or couples who had unused embryos after in vitro fertilization (IVF) procedures. The embryonic stem cells were isolated from the inner cell mass of the blastocyst, a stage in early embryonic development occurring within the first four to six days after fertilization.
The human tissue — typically skin or blood — used to create induced pluripotent stem cell lines is donated by consenting individuals under specific research protocols.
Not all stem cell treatments are approved or proven safe.
A growing number of clinics offer unproven stem cell treatments that have not been evaluated in rigorous clinical trials. These can be costly and, in some cases, dangerous. Before pursuing any stem cell therapy, it's important to ask the right questions.
Find trusted guidance from the ISSCR
For information about stem cell therapies and the availability of stem cell clinical trials at UCLA and beyond, visit our For Patients and Families page.
Want to go deeper?
Explore iPSC research at UCLA
Of all the stem cell types, induced pluripotent stem cells have generated some of the most exciting recent breakthroughs — and UCLA is at the center of that story. See how it all began with our researchers' world-historic 2008 discovery.