Unlocking the potential of patient-derived organoids for personalized sarcoma treatment
Investigators at the UCLA Health Jonsson Comprehensive Cancer Center have developed the largest collection of sarcoma patient-derived organoids to date that can help improve the understanding of the disease and better identify therapies that are most likely to work for each individual patient.
The approach, detailed in the journal Cell Stem Cell, uses patients’ own tumor cells that replicate the unique characteristics of a patient's tumor allowing scientists to quickly screen a large number of drugs in order to identify personalized treatments that can target this rare and diverse group of cancers.
“Sarcoma is a rare and complex disease, which makes conducting clinical trials to identify effective treatments particularly challenging. Some of the rarer subtypes lack standard treatment altogether. Even when multiple therapy options are available, there is often no reliable, data-driven method to determine the best course of action for an individual patient. Choosing the most effective treatment is akin to searching for a needle in a haystack,” said Dr. Alice Soragni, the senior author of the study and assistant professor in the department of Orthopaedic Surgery at the David Geffen School of Medicine at UCLA. “Testing drugs with patient-derived tumor organoids has potential to help predict how a patient may respond to treatment, with the goal of improving patient outcomes for diseases where treatment options are often limited.”
While sarcomas, which can develop in the bones or soft tissues like muscles and adipose tissue, only account for less than 1% of all cancers, they carry a high mortality rate, particularly among young people. The rarity and diversity of sarcoma types—more than 100 distinct subtypes—makes them particularly difficult to study. Responses to conventional therapies can vary widely between patients, making it challenging to determine the most effective course of action for each individual.
To determine whether organoids could enhance the understanding of how a patient’s tumor might respond to specific drugs or combinations, the team assembled a biobank of 294 samples from 126 UCLA patients diagnosed with 25 different subtypes of bone and soft tissue sarcoma. While tumor organoids have been widely used to study carcinomas, this study is the first of its scale to extend organoid development to sarcoma.
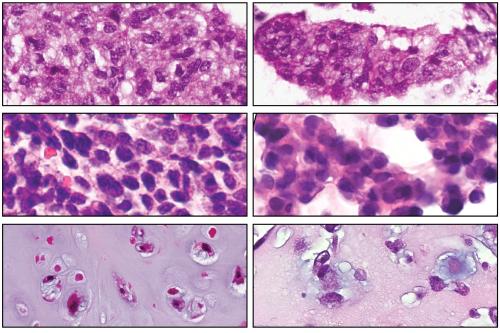
The team successfully created tumor organoids from over 110 samples and conducted detailed histopathological and molecular analyses to confirm that the organoids retained the key characteristics of the original tumors. These organoids were then subjected to high-throughput drug screening using the mini-ring pipeline developed by Soragni and her team, enabling the testing of hundreds of drugs in a 3D format within a short timeframe.
Using this process, the team was able to identify at least one potentially effective U.S. Food and Drug Administration (FDA)-approved treatment for 59% of the samples tested. Additionally, they found the drug responses observed in the lab matched how the patients themselves responded to treatment for a small number of cases, suggesting that these organoids could be a powerful tool for guiding clinical decisions.
“We’ve shown that it’s possible to generate sarcoma organoids quickly —within a week after surgery or biopsy — and use them to screen a large number of drugs, including FDA-approved therapies and other treatments currently in clinical trials,” said Soragni.
“This gives us the ability to identify which drugs are most likely to work for a particular patient, which is crucial for a disease as complex as sarcoma, where genomic precision medicine has often fallen short,” added study author Dr. Noah Federman, the Glaser Family Endowed Chair and director of the UCLA Health Jonsson Comprehensive Cancer Center’s Pediatric Bone and Soft Tissue Sarcoma Program.
In addition, the study demonstrated that a large-scale, functional precision medicine program could be implemented within a single institution, offering a streamlined and scalable model for organoid-based testing.
“Organoids provide a tangible way to match patients with the most promising therapies and this could be a game-changer for sarcoma patients,” said Dr. Nicholas Bernthal, chair and executive medical director of the Department of Orthopaedic Surgery at UCLA. “We’re optimistic that this approach will lead to better, more personalized care for those who need it most.”
Following the results of this study, the UCLA team will validate the findings in a larger clinical trial that is aimed at confirming the effectiveness of the organoid-based approach in predicting treatment responses in patients with osteosarcoma, the most common type of bone cancer that mainly affects children and young adults.
Notes
Soragni, Federman and Bernthal are all members of the UCLA Health Jonsson Comprehensive Cancer Center. The study’s first authors are Ahmad Shihabi, a project scientist in the Soragni laboratory; Peyton Tebon, a visiting project scientist; and Huyen Thi Lam Nguyen, a graduate student. Other UCLA authors are Sara Sartini, Ardalan Davarifar, Alexandra Jensen, Miranda Diaz-Infante, Hannah Cox, Alfredo Enrique Gonzalez, Summer Swearingen, Helena Winata, Sorel Fitz-Gibbon, Takafumi Yamaguchi, Jae Jeong, Sarah Dry, Arun Singh, Bartosz Chmielowski, Joseph Crompton, Fritz Eilber, Scott Nelson, Paul Boutros and Jane Yanagawa.
The study was supported by grants from the National Cancer Institute, the Alan B. Slifka Foundation, David Geffen School of Medicine at UCLA and the UCLA Health Jonsson Comprehensive Cancer Center.

